San Francisco Concussion Injury Attorney — Serious Cases Taken Seriously
Concussions are the most misunderstood injury in personal injury law. Insurance companies routinely dismiss them as “mild” or “minor” — words that do not reflect the medical reality of what happens inside the brain during a concussion, or the serious long-term consequences that can follow. I have recovered millions of dollars for Bay Area concussion victims, including a $6,000,000 settlement and a $2,185,000 settlement in traumatic brain injury cases. I know how to build these cases and how to fight back when insurers try to minimize them.
Call me directly at (415) 851-4557 for a free, no-obligation consultation if you or a loved one suffered a concussion in a car accident, pedestrian accident, bicycle crash, or slip and fall anywhere in San Francisco or the Bay Area. No fee unless I win.
What Is a Concussion?
A concussion is a form of traumatic brain injury — a disruption in the normal function of the brain caused by a bump, blow, jolt to the head, or rapid movement of the head without any direct contact at all. Under CDC guidelines, only one of the following needs to be present to diagnose a traumatic brain injury:
- Any period of loss of consciousness
- Any loss of memory for events immediately before or after the injury
- Neurological deficits such as muscle weakness, balance problems, disrupted vision, or sensory loss
- Any alteration in mental state such as confusion, disorientation, slowed thinking, or difficulty concentrating
A concussion satisfies this definition. Losing consciousness is not required. A normal scan does not rule out injury. Most concussion victims meet several of these criteria — and insurance companies count on them not knowing that.
The human brain contains over 86 billion neurons — nerve cells that communicate through long, slender projections called axons. Damage to those axons, even at the microscopic level, sends consequences cascading through every system the brain controls. Understanding what actually happens to axons during a concussion is the key to understanding why these injuries are serious — and why I build cases that insurers cannot easily dismiss.
“Mild” Traumatic Brain Injury Is a Misnomer
The term “mild traumatic brain injury” is a medical classification. It refers to the mechanism and initial presentation of the injury — not to its impact on your life. Losing cognitive function is not mild. What happens to a person, a career, or a family when the brain stops working as it should is not mild.
I do not take these cases lightly. Not ever.
The Career Impact
Consider what a small cognitive deficit actually means in the real world. A San Francisco tech worker whose processing speed drops by 15% may still function. But that person loses the sharp edge that made them competitive, promotable, and valuable in one of the most demanding job markets in the world. That is not a minor loss. That is a career trajectory permanently altered.
Fatigue — one of the most common and most dismissed concussion symptoms — does not just make you tired. Professionals find their concentration failing before the workday ends. Parents struggle to stay present for their children after a long day. Caregivers run out of capacity long before their shift is done. Everyone who depends on that person feels the loss.
The Personal and Emotional Impact
The emotional toll is perhaps the hardest to quantify and the easiest for insurance companies to dismiss. Irritability that strains a marriage. Anxiety that isolates. Depression that descends without warning on someone who was, before the accident, none of those things. Partners, children, and friends experience a version of grief — mourning someone who is still physically present but no longer quite the same.
These are the cases I handle. These are the losses I fight to recover — not just medical bills and lost wages, but the full human cost of what was taken. When I sit across from an insurance adjuster who wants to settle a “mild” TBI case for nuisance value, I am prepared to put every one of those losses in front of a jury.
You Do Not Need a Blow to the Head to Suffer a Concussion
One of the most important things I tell clients — and juries — is that a concussion does not require direct contact with the head. This surprises many people. It is also exactly the argument insurance companies use to deny valid claims.
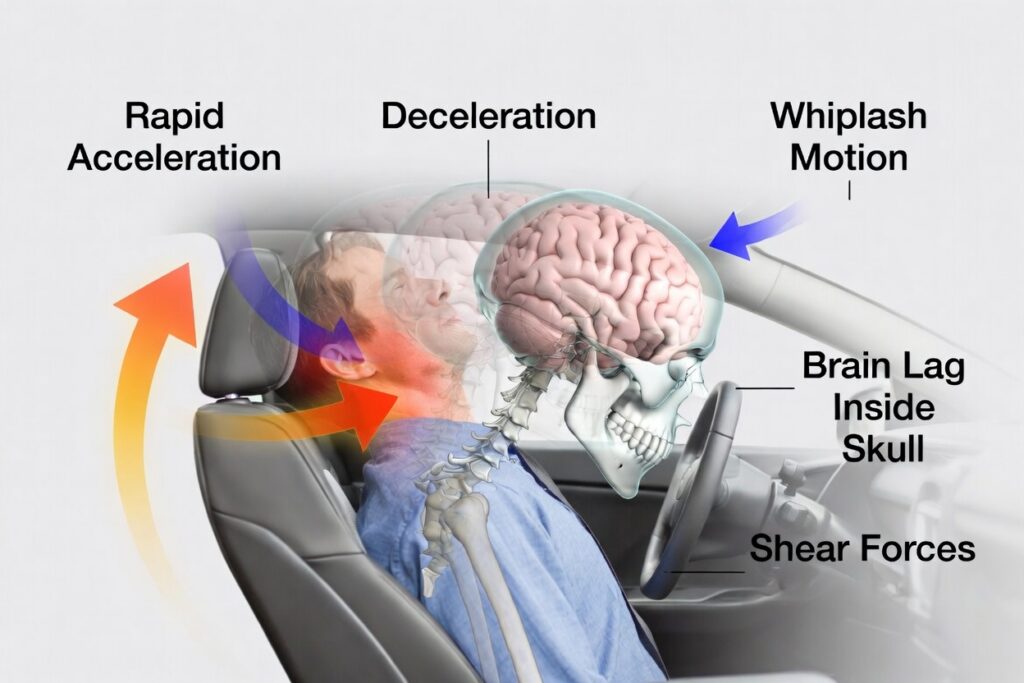
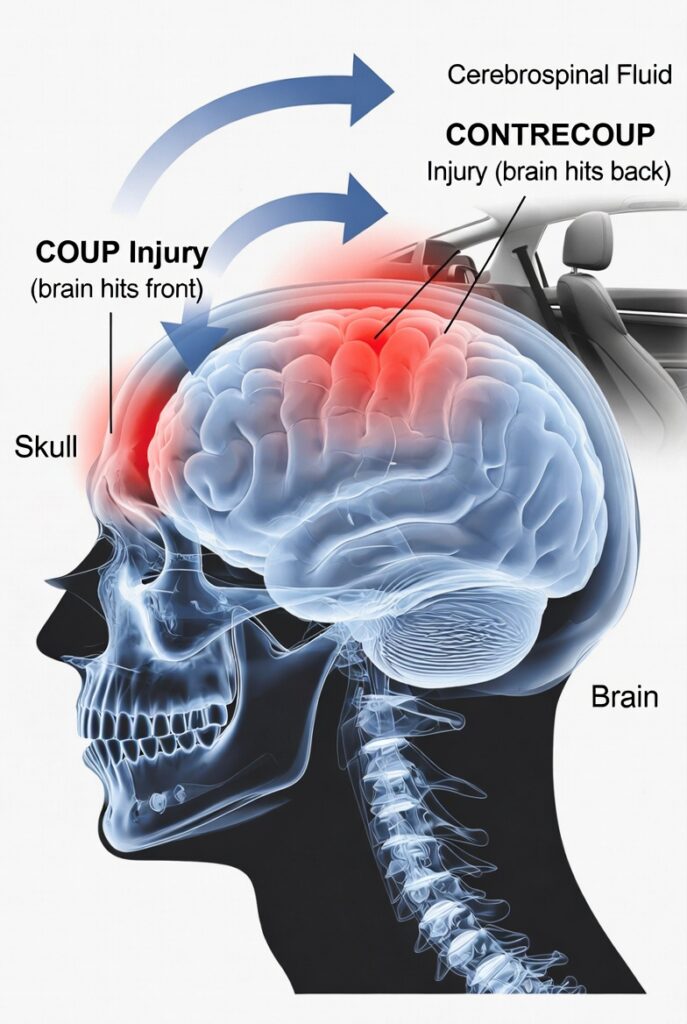
Rapid acceleration and deceleration alone can cause a concussion — the violent whipping of the head forward and backward in a rear-end collision, the sudden rotational force of a T-bone crash, or the abrupt deceleration of a pedestrian struck by a vehicle. The brain, suspended in cerebrospinal fluid inside the skull, does not move at the same speed as the skull during sudden impact. The skull accelerates. The brain lags behind. Then the brain crashes against the interior of the skull as the skull decelerates.
This is the coup-contrecoup mechanism: the brain sustains injury at the point of initial impact inside the skull (coup), and again on the opposite side as it rebounds (contrecoup). Two separate injury locations. No external blow to the head required.
What Is an Axon — and What Happens to It in a Concussion?
The Brain’s Communication System
To understand why concussions are serious, you need to understand what is happening at the cellular level inside the brain.
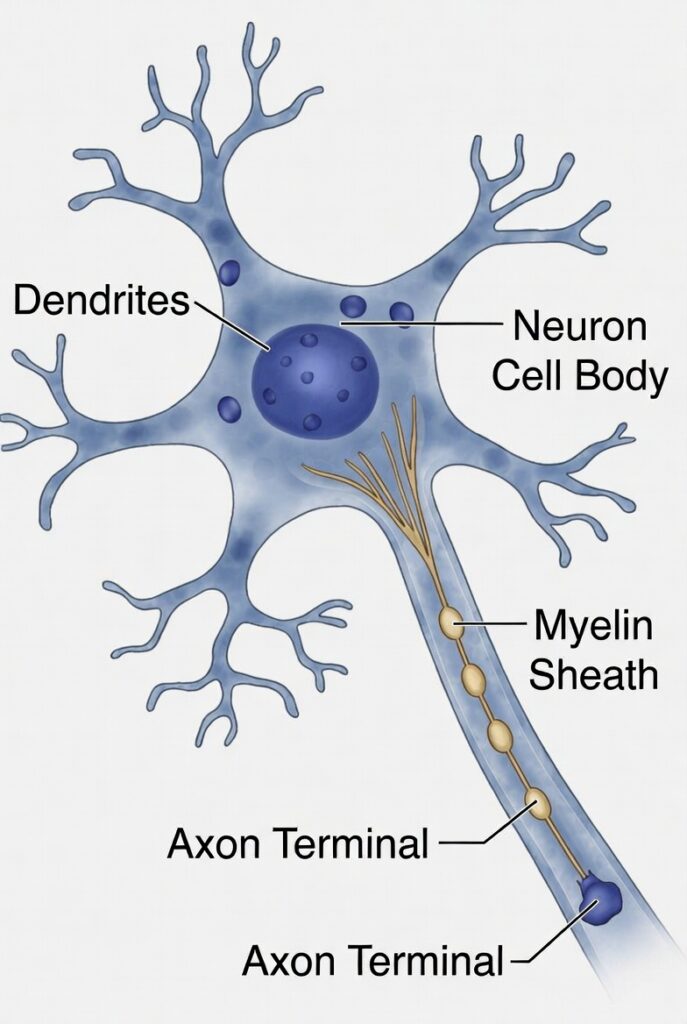
An axon is the long, slender projection of a nerve cell (neuron) that carries electrical signals from one neuron to the next. Think of axons as the communication cables of the brain — organized bundles running through the brain’s white matter that allow different regions to talk to each other. Every thought, memory, movement, and emotion depends on axonal signaling.
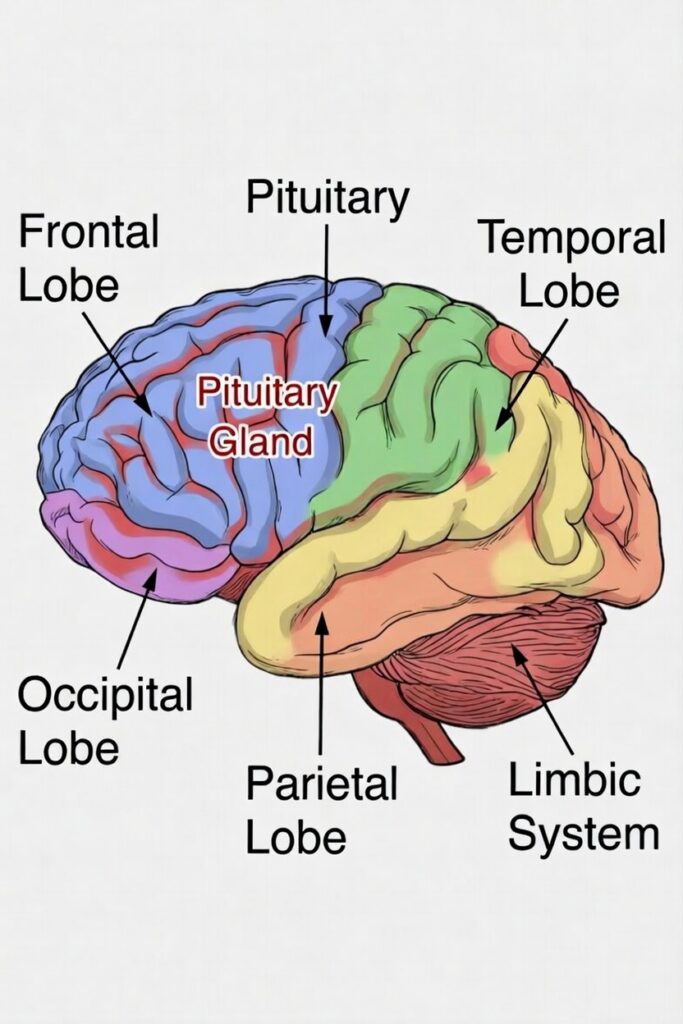
The brain divides into left and right hemispheres, each containing four lobes. The frontal lobe governs personality, executive function, and decision-making. The temporal lobe handles memory and language. The parietal lobe processes sensory information and spatial awareness. The occipital lobe controls vision. The limbic system governs emotion and memory. The pituitary gland controls the body’s hormonal systems. Axonal injury in any of these regions disrupts the specific functions that region controls — which is why concussion symptoms vary so widely from person to person.
Under normal conditions, axons are remarkably elastic. They can stretch to twice their resting length and spring back undamaged. Rapid, high-force acceleration or rotation changes everything.
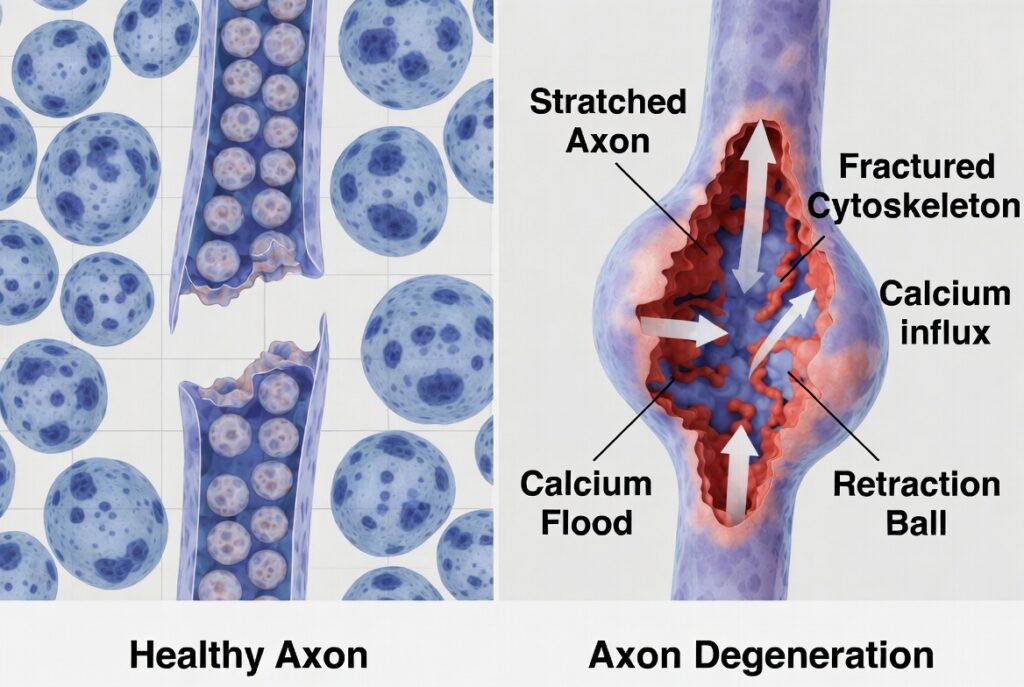
What High-Force Impact Does to an Axon
The axonal cytoskeleton fractures. The internal scaffolding of the axon — made of proteins called neurofilaments and microtubules — physically breaks under tensile and shear forces. The axon does not snap cleanly like a wire. The cytoskeleton cracks at the point of maximum stress.
Calcium floods into the cell. The mechanical disruption tears open ion channels in the axon membrane. Sodium rushes in. Voltage-gated calcium channels open. Calcium ions flood the cell, triggering a destructive biochemical cascade that damages mitochondria, degrades the cytoskeleton further, and kills the neuron from within.
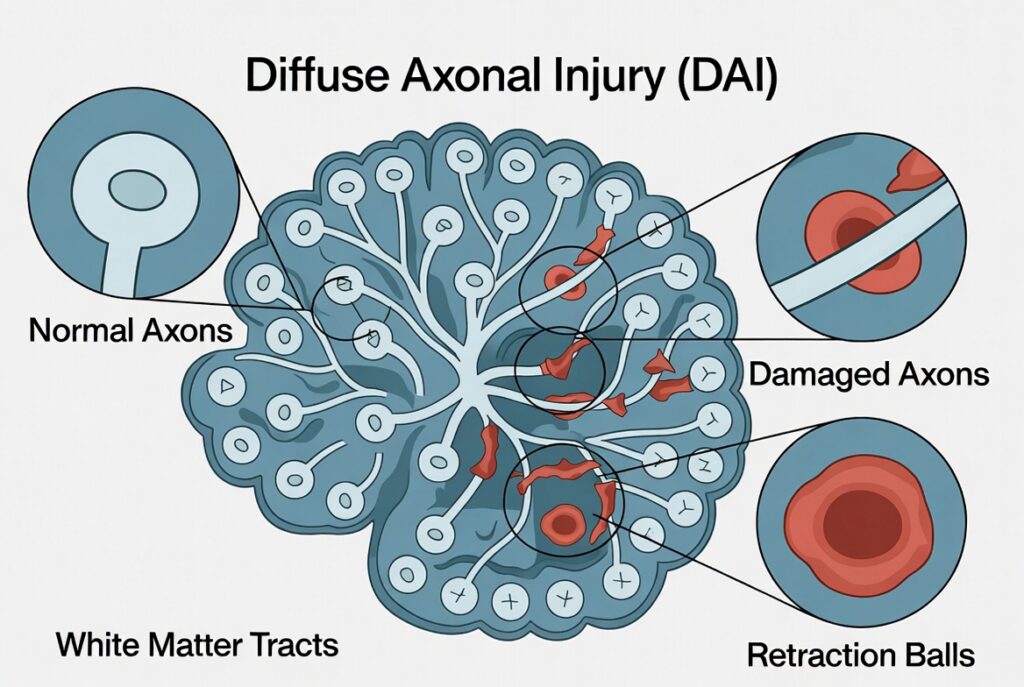
Axonal transport breaks down. Axons constantly transport proteins and nutrients from the cell body to the axon tip. When the cytoskeleton breaks, this transport system jams. Materials pile up at the break point, causing the axon to swell into a visible bulge called a retraction ball — the histological hallmark of diffuse axonal injury.
The axon severs and degenerates. Once the swelling grows large enough, the axon tears at the break point. The segment beyond the tear degrades and dies in a process called Wallerian degeneration, beginning within 24 to 48 hours and continuing for months.
Why This Damage Is Often Invisible
CT scans — the most commonly used imaging after accidents — cannot detect axonal injury. The damage occurs at the microscopic level, far below CT resolution. A normal CT scan does not mean no brain injury occurred. Advanced MRI with diffusion tensor imaging (DTI) reveals white matter damage that standard scans miss entirely.
This process — widespread axonal damage across multiple brain regions from rapid acceleration forces — is Diffuse Axonal Injury (DAI). Concussion now represents the milder end of the DAI spectrum. The same mechanism that causes a concussion, applied with greater force or duration, causes severe traumatic brain injury.
How Concussions Happen in San Francisco Accidents
Any accident causing sudden acceleration, deceleration, or rotation of the head can cause a concussion. In San Francisco, I see these mechanisms most often:
Common San Francisco Accident Mechanisms
Rear-end car accidents — The whiplash motion snaps the head forward and backward, subjecting the brain to rapid deceleration forces. Even low-speed rear-end collisions cause concussion through this mechanism.
T-bone and intersection collisions — Lateral impact causes rotational acceleration of the brain — one of the most damaging mechanisms for axonal injury. San Francisco’s most dangerous intersections — Market and Octavia, Van Ness and Market, 5th and Market — see these crashes regularly.
Pedestrian accidents — A pedestrian struck by a vehicle undergoes sudden violent acceleration followed by impact with the ground or vehicle. My pedestrian TBI results include a $6,000,000 settlement and a $2,185,000 settlement.
Bicycle accidents — Even with a helmet, a cyclist thrown from their bike can suffer significant concussive injury from the rapid deceleration of impact with the ground or vehicle.
Slip and fall accidents — Falling onto a hard surface — a concrete sidewalk, a tile floor, a staircase — causes sudden impact deceleration. San Francisco’s aging sidewalks and steep hills make these falls especially dangerous.
Muni and BART accidents — Sudden braking, jolting stops, and collisions aboard public transit vehicles subject passengers to significant acceleration-deceleration forces without any external blow to the head.
Concussion Symptoms — What to Watch For
One of the most dangerous aspects of concussion is that symptoms do not always appear immediately. The biochemical cascade that damages axons unfolds over hours and days after injury. Feeling fine at the scene of an accident does not mean you were not injured — serious symptoms can develop later that day, the next morning, or several days afterward. Never assume a symptom-free moment after a crash means you escaped injury.
Concussion symptoms fall into four categories:
Physical and Sensory
Headache or pressure in the head, nausea or vomiting, dizziness, balance problems, sensitivity to light (photophobia), sensitivity to noise (phonophobia), ringing in the ears (tinnitus), blurred or double vision, fatigue, post-traumatic migraine appearing up to seven days after injury.
Cognitive
Feeling mentally foggy or slowed down, difficulty concentrating, memory problems — particularly for events immediately before or after the accident — confusion, disorientation.
Emotional and Mood
Irritability, sadness, anxiety, increased emotionality, mood swings, feeling unlike yourself without a clear explanation.
Sleep
Sleeping significantly more or less than usual, difficulty falling asleep, disrupted sleep patterns.
When to Seek Emergency Care Immediately
Most concussion symptoms develop gradually. Some symptoms signal a potentially life-threatening emergency requiring immediate 911 or emergency room care:
- Worsening headache that intensifies over time rather than improving
- Repeated vomiting
- Seizures
- Slurred speech
- One pupil larger than the other
- Extreme drowsiness or inability to wake up
- Increasing confusion or unusual behavior
- Weakness or numbness in arms or legs
These symptoms can indicate a more serious brain injury — including a subdural or epidural hematoma — requiring urgent surgical intervention. Do not wait. Call 911.
Document Your Symptoms From Day One
Document symptoms from the moment they appear, whether mild or severe. Keep a daily symptom journal — date, time, what you felt, how long it lasted, how it affected your activities. Note the first time you mention symptoms to a family member or friend. Their recollection of that conversation becomes evidence. Track any changes in work performance, sleep, mood, or relationships.
This documentation forms part of the story I tell on your behalf — corroborated by the people around you who noticed the change before you fully understood what was happening.
Seek medical attention immediately after any accident where you experience any of these symptoms — even minor ones. The medical record created by that visit is the foundation of your concussion claim.
💡Pro Tip from Attorney John J. Roach
Keep a daily concussion symptom journal starting the day of your accident. Record the date, time, what you experienced, how long it lasted, and how it affected your work, relationships, and daily activities. Note every time you mention symptoms to a family member, friend, or coworker — their recollection becomes evidence. Bring the journal to every medical appointment. This record is one of the most powerful tools I use to build concussion cases that insurance companies try to dismiss.
Why a Normal ER Visit Does Not Mean You Were Not Injured
What the ER Is Actually Designed to Find
Emergency rooms exist to rule out life-threatening emergencies. Doctors look for skull fractures, brain bleeds, and surgical emergencies. An ER physician who documents “no acute intracranial abnormality” on a CT report is communicating one thing: you do not need brain surgery. That note says nothing about whether your brain sustained injury.
Most concussion cases I handle follow the same pattern. The client went to the ER after their accident, received a normal CT scan, heard instructions to rest and follow up with a doctor, and then left with a discharge sheet. No concussion diagnosis. No neurologist referral. No neuropsychological testing.
Insurance companies treat that ER visit as the end of the story. I treat it as the beginning.
CT scans and standard MRIs cannot detect diffuse axonal injury. The microscopic damage to axons occurs at a cellular level — far below the resolution of standard imaging. A normal scan is not evidence of no injury. These tools were never designed to find this type of injury.
The Best Witnesses Are the People Who Know You
In nearly every concussion case I handle, the clearest evidence of injury does not come from a scan. It comes from the people closest to the client. A spouse who notices their partner is short-tempered and withdrawn for the first time in 20 years of marriage. A supervisor who sees a previously sharp employee missing deadlines and struggling to follow instructions. A parent who notices their child’s personality has shifted since the accident. A close friend who says simply: “That’s not the person I know.”
I gather these observations through careful interviews, written statements, and deposition testimony. Juries understand them immediately. No medical degree is required to grasp that a person has changed. These stories make concussion cases real to a jury in a way that imaging reports cannot.
Objective Testing Fills the Gap
A neuropsychologist administers a battery of standardized cognitive tests measuring memory, processing speed, attention, executive function, and verbal fluency — the exact functions that axonal injury disrupts. These tests produce objective, quantified results. When testing shows that a client’s processing speed ranks at the 15th percentile compared to pre-injury norms, that is not a subjective complaint. That is a measurable, documented deficit.
Neurologists Make the Diagnosis
A neurologist who examines the client, reviews the imaging, takes a thorough history, and correlates the clinical picture with the accident mechanism can render the diagnosis the ER never made. The neurologists I work with understand concussion and diffuse axonal injury. They explain the coup-contrecoup mechanism in terms a jury can follow. They connect the client’s current symptoms directly to the accident.
Family and friend testimony, neuropsychological test results, and neurologist diagnosis — that combination is how I prove concussion cases that insurance companies initially dismissed as having “no objective findings” — and recover full and fair compensation for my clients.
The Long-Term Effects of Concussion
Medical science does not support the insurance industry narrative that concussions are minor injuries resolving quickly.
Post-Concussion Syndrome
Post-Concussion Syndrome (PCS) affects up to 20% of concussion victims. Symptoms persist for months or years beyond the initial injury. For some victims they never fully resolve.
Cognitive and Emotional Effects
Cognitive impairment — difficulties with memory, processing speed, executive function, and attention — can persist long after visible symptoms resolve. Work performance suffers. Quality of life suffers. These losses are difficult to quantify but real and compensable.
Depression, anxiety, PTSD, and personality changes are direct consequences of concussion that research documents clearly. The same biochemical disruption that damages axons also disrupts the brain’s emotional regulation systems. Insurers call these psychological — I call them neurological, and I prove it.
Overlooked Consequences
Pituitary injury is one of the most frequently overlooked concussion consequences. The pituitary gland — which regulates the body’s hormonal systems — sits at the base of the brain. The same acceleration-deceleration forces that cause concussion threaten it too. Traumatic hypopituitarism causes profound fatigue, depression, cognitive impairment, weight changes, and sexual dysfunction. Doctors frequently misdiagnose these symptoms as psychological in origin. Treating physicians and opposing experts routinely miss this injury. I work with endocrinologists and neuroendocrinologists to identify and document pituitary damage in my cases.
Rare but Serious Long-Term Risks
Second Impact Syndrome occurs when a second concussion strikes before the first has fully healed. The result can be catastrophic, potentially fatal brain swelling. The brain is uniquely vulnerable during concussion recovery.
Chronic Traumatic Encephalopathy (CTE) — a progressive neurodegenerative disease linked to repeated brain trauma — causes tau protein accumulation in the brain. Progressive cognitive decline, behavioral changes, depression, and dementia follow. CTE strikes anyone who suffers repeated concussive injuries — not only athletes.
Growing scientific evidence shows that even a single concussion can push the brain onto an accelerated neurodegenerative path. Disruption of axonal transport systems and accumulation of amyloid precursor protein at injury sites mirror the pathological changes in Alzheimer’s disease.
Why Insurance Companies Fight Concussion Claims — and How I Fight Back
“The CT scan was normal.” Standard CT imaging cannot detect diffuse axonal injury. A normal CT is not evidence of no injury. I counter this with advanced MRI including DTI, neuropsychological testing, and expert neurologist testimony.
“There was no loss of consciousness.” Loss of consciousness is absent in the majority of concussion cases. Under CDC guidelines, only one of four criteria needs to be present — and LOC is just one of them.
“The impact was too minor to cause a brain injury.” Low-speed collisions cause concussions through the coup-contrecoup mechanism. Biomechanical experts and neurologists help me establish the mechanism and connect it to the client’s symptoms.
“The symptoms are subjective.” Neuropsychological testing objectively measures cognitive deficits. Daily limitation documentation from family members and employers adds corroboration. Life care plans from qualified experts quantify ongoing costs.
“The symptoms are pre-existing.” Insurance companies comb through medical history looking for prior headaches, anxiety, or cognitive complaints. Careful record review and expert testimony establish the causal link between the accident and the client’s current condition.
My Results in Brain Injury and Concussion Cases
Insurance companies know I take concussion cases to trial when necessary. That preparation drives better settlements.
- $6,000,000 — Settlement for a pedestrian struck by a vehicle who suffered a traumatic brain injury
- $2,185,000 — Settlement in another traumatic brain injury case (pedestrian vs. auto)
- $750,000 — UIM arbitration award for mild traumatic brain injury from a rear-end collision — far exceeding the insurer’s initial offer, after proving long-term cognitive and emotional impacts through expert evidence
- $425,000 — Settlement for slip and fall with disputed liability involving mild traumatic brain injury
Results in prior cases do not guarantee a similar outcome in your case. Every case is unique and depends on its specific facts, injuries, and insurance coverage.
Common Questions About Concussion Injury Claims in San Francisco
Yes. A concussion does not require direct contact with the head. The rapid acceleration and deceleration forces in a car accident — particularly rear-end and T-bone collisions — can cause the brain to move violently inside the skull, injuring axons through the coup-contrecoup mechanism. I regularly represent clients who suffered concussions in rear-end crashes where their head never struck anything.
A normal CT scan does not mean you did not suffer a concussion. Standard CT imaging cannot detect diffuse axonal injury — the microscopic damage to axons that is the hallmark of concussion. I build concussion cases using advanced MRI imaging, neuropsychological testing, and expert neurologist testimony that explains why imaging limitations are not evidence that no injury occurred.
Most concussion symptoms resolve within days to weeks. However up to 20% of concussion victims develop Post-Concussion Syndrome — persistent symptoms that can last months or years. Long-term consequences including cognitive impairment, pituitary injury, depression, and in cases of repeated concussions, chronic traumatic encephalopathy (CTE), are well-documented in the medical literature.
The value of a concussion claim depends on the severity of symptoms, duration of recovery, impact on work and daily life, and available insurance coverage. I have recovered $750,000 for a mild TBI victim in a rear-end collision and $425,000 in a slip and fall concussion case with disputed liability. I offer free consultations to give you an honest assessment of what your specific case may be worth.
Yes — immediately, even if you feel relatively fine. Many concussion symptoms are delayed, appearing hours or days after injury as the biochemical damage to axons unfolds. The medical records created by that visit are critical evidence in your claim. A gap between your accident and your first medical visit is one of the primary tools insurance adjusters use to deny concussion claims.
Generally two years from the date of your injury. However if a government entity is involved — such as the City of San Francisco, BART, or Muni — you may have as little as six months to file a government tort claim. Contact me immediately after your accident — delays can permanently bar your recovery.
Contact a San Francisco Concussion Injury Attorney Today
Concussion cases require an attorney who understands the medicine, anticipates the insurance tactics, and knows how to present complex brain injury evidence to a jury. I have recovered millions of dollars for Bay Area brain injury victims — including a $750,000 result for a mild TBI in a rear-end collision — by treating every concussion case with the seriousness the injury deserves.
Call me directly at (415) 851-4557 or fill out the free consultation form here. I answer the phone personally. Available in English and Spanish. No fee unless I win.
